Parkinson’s care at home is a deeply personal journey—one that often begins quietly and evolves over time.
At first, the changes may feel small. A slight tremor. A slower step. A moment of hesitation before standing up. These early signs can be easy to adapt to, and life may continue much as it always has.
But Parkinson’s disease is progressive. As it advances, care at home often becomes more complex—affecting not only physical health, but emotional well-being, daily routines, and long-term planning.
If you are navigating Parkinson’s care at home, you are not alone.
Millions of families across the United States are caring for someone with Parkinson’s, balancing love, responsibility, and uncertainty. This guide is here to help you understand what to expect, how care needs evolve, and when it may be time to explore additional support.
What Is Parkinson’s Disease?
Parkinson’s disease is a chronic, progressive neurological condition that affects movement, coordination, and, in some cases, thinking and memory.
It develops when nerve cells in the brain that produce dopamine—a chemical responsible for smooth, controlled movement—begin to deteriorate over time. As dopamine levels decrease, movement becomes slower, less coordinated, and more difficult to control.
According to the Parkinson’s Foundation, nearly one million people in the United States are living with Parkinson’s disease—and that number is expected to grow.
For families, understanding how Parkinson’s affects the body is an important first step in understanding how care needs may change over time.
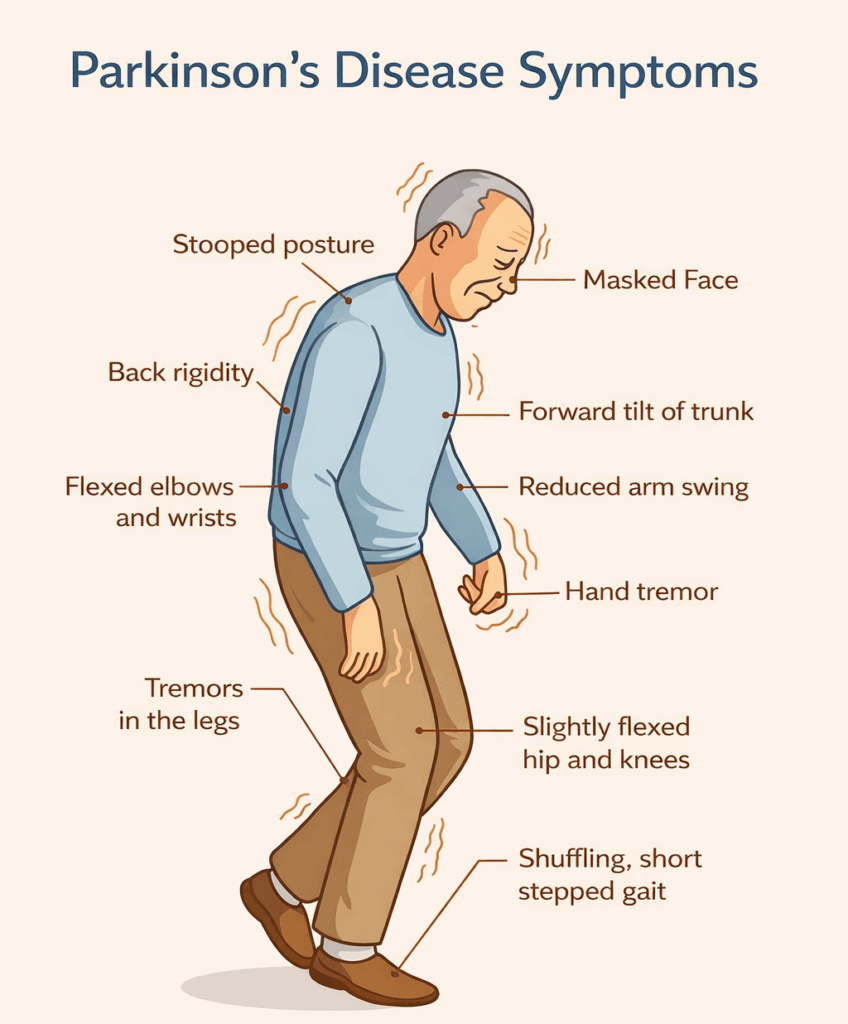
Common Symptoms of Parkinson’s Disease
Parkinson’s symptoms are often grouped into two categories: motor symptoms (those that affect movement) and non-motor symptoms (those that affect mood, thinking, and overall well-being).
Motor Symptoms
- Tremors, often starting in one hand
- Slowed movement (bradykinesia)
- Muscle stiffness
- Balance and coordination challenges
Non-Motor Symptoms
- Depression and anxiety
- Sleep disturbances
- Cognitive changes
- Fatigue
- Constipation
These symptoms tend to develop gradually, which is why caregiving needs often increase slowly—rather than all at once.
Understanding Parkinson’s Disease Progression
Parkinson’s disease progression is not always predictable. Some individuals experience slow changes over many years, while others may notice symptoms becoming more pronounced more quickly.
Healthcare professionals may describe Parkinson’s in stages, but for families, it is often more helpful to focus on how care needs evolve over time.
Early Stage: Subtle but Meaningful Changes
In the early stage, symptoms are often mild, and many individuals continue to live independently.
You may notice small changes—slight tremors, subtle shifts in posture, or increased fatigue. Daily routines are still largely intact, but small adjustments may begin to appear.
At this stage, caregiving often involves emotional support, encouragement to stay active, and simply paying attention to how things are changing.
This is also an important time to begin thinking ahead. Exploring care options early can make future decisions feel more manageable—especially when you understand how to plan before a crisis happens.
Middle Stage: Increasing Support Needs
As Parkinson’s progresses, changes become more noticeable and begin to affect daily life more directly.
Movement may become slower and more rigid. Balance may decline. Tasks that once felt simple may take more time and effort.
Caregiving responsibilities often expand to include help with daily activities, medication management, and mobility support. This stage often marks the transition from occasional assistance to more consistent, daily caregiving.
Advanced Stage: Complex, Full-Time Care
In later stages, care needs can become significantly more intensive.
Mobility may be severely limited. Assistance may be needed for most daily activities. Cognitive changes or dementia may also develop.
At this point, caregiving may require full-time support, increased supervision, and more advanced care planning.
Understanding these changes can help families prepare—not just physically, but emotionally.
Parkinson’s Disease Stages: What to Expect Over Time
Understanding how Parkinson’s disease progresses can help families anticipate changes and make more confident decisions.
While every experience is different, the table below provides a helpful overview of how symptoms and care needs often evolve:
| Stage | What You May Notice | Independence | Care Needs |
| Early | Mild symptoms, subtle changes | Mostly independent | Occasional support |
| Middle | Balance issues, slower movement | Partial independence | Daily assistance |
| Advanced | Severe limitations, cognitive changes | Limited independence | Full-time care |
Daily Life: What Care Looks Like at Home
As Parkinson’s disease progresses, Parkinson’s care at home begins to shift in quiet but meaningful ways.
Simple routines—getting dressed, preparing meals, or walking across a room—may take more time, require more patience, and eventually call for more support.
Over time, caregiving becomes less about occasional help and more about ongoing support throughout the day.
Mobility Challenges and Fall Risk
Mobility changes are often one of the most noticeable aspects of Parkinson’s—and one of the most important to address early. You may begin to notice changes in walking patterns, balance, and coordination. These changes can increase the risk of falls.
According to the Centers for Disease Control and Prevention, falls are a leading cause of injury among older adults.

Making the Home Safer
Simple changes can make a meaningful difference:
- Remove loose rugs and clear clutter from walkways
- Install grab bars in bathrooms and near stairs
- Improve lighting, especially in hallways and entryways
- Use mobility aids such as walkers or canes when needed
- Consider physical or occupational therapy for movement support
These adjustments are not just about safety—they help preserve confidence and independence. In many cases, thoughtful home modifications can also extend the ability to remain at home longer before transitioning to additional care.
Medication Management: A Critical Part of Parkinson’s Care
Medication management is one of the most important—and often most challenging—parts of caring for someone with Parkinson’s disease at home.
Unlike many other conditions, Parkinson’s medications are highly time-sensitive. They must be taken at specific times each day to help maintain movement, reduce symptoms, and support overall function.
Even a small delay or missed dose can lead to noticeable changes, including:
- Increased stiffness
- Slowed or limited movement
- Greater difficulty walking or standing
- Increased risk of falls
These moments—when medication is not working as effectively—are often referred to as “off” periods. They can feel frustrating and unpredictable, both for your loved one and for you as a caregiver.
Over time, keeping medications consistent often becomes one of the most structured—and demanding—parts of the day.
Medication Mistakes to Avoid
Managing Parkinson’s medications can feel overwhelming, especially as schedules become more complex. Even small inconsistencies can affect how well medications work and how your loved one feels throughout the day.
Being aware of common challenges can help you stay one step ahead—and prevent unnecessary stress.
Common Medication Mistakes to Watch For
- Missing doses or taking them late
Even short delays can trigger “off” periods, leading to stiffness and difficulty moving - Inconsistent timing from day to day
Parkinson’s medications work best when taken at the same times every day - Not coordinating medications with meals
Some medications are affected by food—especially protein—or need to be taken on an empty stomach. Always follow medical guidance - Accidentally skipping or doubling doses
This can happen easily without a clear system in place, particularly as schedules become more frequent - Not tracking symptom changes or side effects
Changes in movement, mood, or behavior may be connected to medication timing or dosage - Trying to manage everything alone when it becomes too complex
As care needs increase, doing it all without support can lead to stress and a higher risk of mistakes
If this feels familiar, you are not alone—many caregivers find that medication schedules gradually become one of the most structured parts of the day.
Simple Ways to Stay on Track
Small, consistent systems can make a meaningful difference in keeping medications organized and manageable:
- Use a weekly pill organizer
- Set alarms or phone reminders for each dose
- Keep a written medication schedule in a visible place
- Track symptoms and share updates with healthcare providers
- Ask for help when routines become difficult to manage
These simple tools not only improve consistency—they can also reduce daily stress and give you more confidence in your caregiving routine.
If medication management is starting to feel overwhelming, it may be a sign that additional support could help. This is not a failure—it is a natural part of how Parkinson’s care evolves over time.
Nutrition, Swallowing, and Weight Changes
As Parkinson’s disease progresses, it can begin to affect the muscles used for chewing and swallowing—a condition known as dysphagia.
These changes often develop gradually, but they can have a meaningful impact on nutrition, safety, and overall well-being.
Signs to Watch For
You may begin to notice:
- Coughing or choking during meals
- Difficulty swallowing certain foods or liquids
- Eating more slowly or avoiding meals
- Unintended weight loss
Supportive Strategies
There are simple, supportive ways to make meals safer and more comfortable:
- Offer soft foods or modified textures that are easier to chew and swallow
- Encourage slow eating with small bites and sips
- Ensure your loved one is sitting upright during meals—and for a short time afterward
- Minimize distractions so they can focus while eating
- Consult a speech-language pathologist if swallowing difficulties increase
Small adjustments like these can make a meaningful difference—not only in safety, but also in confidence and comfort during meals.
Foods to Avoid vs. Foods That Help
Understanding which foods are easier—or more difficult—to manage can make mealtimes safer, more comfortable, and less stressful.
Small changes in texture and consistency can have a meaningful impact on both safety and overall eating experience.
| Foods to Be Cautious With | Why They Can Be Difficult | Foods That May Help | Why They Are Easier |
| Dry, crumbly foods (crackers, toast, cookies) | Hard to chew and may increase choking risk | Soft foods (mashed potatoes, yogurt, applesauce) | Easier to swallow and require less chewing |
| Tough meats (steak, pork chops) | Require more chewing and can be difficult to swallow | Tender proteins (ground meat, fish, shredded chicken) | Softer texture makes swallowing easier |
| Sticky foods (peanut butter, thick bread) | Can stick in the throat and increase choking risk | Moist foods (soups, stews, casseroles) | Added moisture helps food go down more smoothly |
| Thin liquids (water, juice, coffee) | May be harder to control when swallowing | Thickened liquids (as recommended by a professional) | Easier to control and safer for swallowing |
| Mixed textures (cereal with milk, chunky soups) | Different consistencies can be difficult to manage | Smooth or uniform textures (pureed foods, blended soups) | More predictable and easier to swallow safely |
A Helpful Note
Every person’s needs are different, and swallowing challenges can change over time.
If you notice ongoing difficulty with eating or drinking, a healthcare provider or speech-language pathologist can recommend adjustments tailored to your loved one’s specific needs.
One caregiver shared that simply changing the texture of meals made a noticeable difference—not only in safety, but in how relaxed and comfortable mealtimes began to feel again.
Why Nutrition Matters
Good nutrition plays an essential role in maintaining strength, energy, and overall well-being.
When eating becomes difficult, it is not just about food—it can affect independence, confidence, and overall quality of life.
Addressing these changes early can help your loved one stay healthier and more comfortable, while also reducing stress around mealtimes—for both of you.

Sample 1-Day Meal Plan for Parkinson’s Care
Planning meals can feel overwhelming when swallowing or appetite changes become part of daily life. Having a simple structure can make it easier to ensure your loved one is getting the nutrition they need—without adding extra stress to your day.
Here’s an example of a gentle, easy-to-manage daily meal plan:
Daily Meal Plan Overview
| Time of Day | Meal Ideas |
| Breakfast | Oatmeal with mashed banana Scrambled eggs (soft texture) Yogurt Warm tea or a thickened beverage (if recommended) |
| Mid-Morning Snack | Applesauce or soft fruit puree Smoothie (blended fruit with yogurt or a milk alternative) |
| Lunch | Creamy vegetable soup or blended soup Soft bread or well-moistened grains Cottage cheese or another soft protein option |
| Afternoon Snack | Pudding or yogurt Soft fruit (such as ripe banana or peaches) |
| Dinner | Baked or poached fish (soft and flaky) Mashed potatoes or soft rice Steamed vegetables (well-cooked and soft) |
| Evening Snack (if needed) | Warm milk or a thickened beverage Soft snack such as pudding or applesauce |
This sample plan can be adjusted based on your loved one’s preferences, nutritional needs, and swallowing ability.
A Gentle Reminder
Food preferences, tolerance, and swallowing ability can change over time.
Some individuals may need more texture modification, while others may tolerate a wider range of foods. If swallowing becomes more difficult, a speech-language pathologist can help guide safe food and liquid choices.
Even small adjustments—like adding moisture, softening textures, or spacing meals throughout the day—can make eating safer, more comfortable, and more enjoyable.
As nutritional needs evolve, you may also begin to notice changes beyond physical health—particularly in memory, thinking, and overall behavior.
Cognitive Changes and Parkinson’s Disease Dementia
While Parkinson’s disease is often recognized for its impact on movement, it can also affect thinking, memory, and behavior—especially as the disease progresses.
According to the National Institute on Aging, some individuals with Parkinson’s may develop Parkinson’s disease dementia, a condition that can gradually change how a person thinks, communicates, and interacts with the world around them.
These changes can feel subtle at first, but over time, they may become more noticeable in everyday life.
Symptoms May Include:
- Memory loss or increasing forgetfulness
- Confusion or disorientation
- Difficulty focusing or following conversations
- Changes in mood, behavior, or personality
- Hallucinations in some cases
These symptoms often develop gradually, but they can have a meaningful impact on daily routines, communication, and overall safety.
What This Means for Families
Cognitive changes can be especially challenging—not only because of the symptoms themselves, but because they affect how you connect and communicate with your loved one.
You may find that:
- Conversations become more difficult or require more patience
- Daily routines need more structure and consistency
- Supervision becomes increasingly important
- Your loved one may seem different in ways that are hard to understand or process
For many families, this stage can feel overwhelming.
It is important to remember that needing additional support at this point is not uncommon—it is often a natural part of how care needs evolve over time.
When More Specialized Care May Be Needed
As cognitive symptoms progress, care often becomes more specialized. Structured environments—such as memory care—can provide a safer and more supportive setting for individuals experiencing cognitive decline.
They can offer:
- Safer, more predictable surroundings
- Staff trained in dementia care
- Consistent routines designed to reduce confusion and anxiety
Recognizing these changes early can help you explore options thoughtfully, giving you time to make decisions with clarity rather than urgency. If you would like to better understand how memory care works and what it provides, you can explore our guide: Memory Care Explained: A Complete Guide for Families Navigating Alzheimer’s and Dementia Care
The Emotional Reality of Caregiving
Caring for someone with Parkinson’s disease is not only a physical responsibility—it is an emotional journey as well.
As the disease progresses, you may find yourself navigating a wide range of feelings, sometimes all at once.
You may experience:
- Grief as you watch your loved one change over time
- Stress from the ongoing responsibility of caregiving
- Guilt for feeling overwhelmed or needing help
- Physical and emotional exhaustion
These feelings are not only common—they are completely valid.
For many caregivers, the emotional weight builds gradually. What begins as small adjustments can slowly become a constant presence in daily life.
Caregiver burnout is real, and it can affect your health, your energy, and your ability to continue providing care.
Taking care of yourself is not separate from caregiving—it is an essential part of it.
Reaching out for support, taking breaks when possible, and recognizing your own limits are not signs of weakness. They are part of sustaining the care and compassion you are already giving every day.

And perhaps most importantly, you are not alone in feeling this way—many caregivers walk this same path, even if it doesn’t always feel visible.
When Care at Home Becomes More Difficult
There is rarely a single moment when everything changes.
Instead, Parkinson’s care at home often becomes more demanding little by little—until one day, it begins to feel overwhelming.
Recognizing these changes early can help you make thoughtful, informed decisions—rather than feeling forced to act during a crisis.
Signs It May Be Time for Additional Support
You may begin to notice:
- Frequent falls or increasing safety concerns
- Difficulty managing medications on time
- Growing dependence for daily activities like bathing, dressing, or eating
- Cognitive changes, confusion, or memory loss
- Physical or emotional exhaustion as a caregiver
If several of these signs are present, it may be time to consider additional support—especially if daily care needs are becoming difficult to manage at home.
If you are starting to wonder when it might be time to consider assisted living, this guide can help you recognize the signs: When Is It Time for Assisted Living? 12 Signs an Older Adult May Need More Support
Exploring Long-Term Care Options
As care needs increase, many families begin exploring options that can provide additional support, safety, and peace of mind.
Understanding what each option offers can help you choose what feels right for your loved one—and for you.
In-Home Care
Provides non-medical assistance while allowing your loved one to remain at home. This may include help with personal care, daily tasks, and companionship.
Home Health Care Offers medical support at home, such as nursing care, physical therapy, and medication management—often following an illness or hospitalization.
Assisted Living Provides a supportive community environment with help for daily activities, meals, and 24-hour staff availability.
Memory Care Designed for individuals experiencing dementia or cognitive decline, with secure environments and specialized, structured support.
Residential Care Homes Smaller, home-like settings that offer more personalized care and a quieter environment.
Nursing Homes (Skilled Nursing) Provide 24/7 medical care and supervision for individuals with complex or advanced health needs.
Hospice Care Focuses on comfort, dignity, and quality of life for individuals with serious or terminal illness. Hospice care can be provided at home, in hospice centers, or within other care settings, offering physical, emotional, and spiritual support for both the individual and their family.
Hospice care is different from long-term care because it focuses on comfort rather than ongoing support or rehabilitation, but it is still an important part of the care journey for many families.
Taking the Next Step
If you are beginning to explore care options, you do not have to navigate this alone. You can search, compare, and connect directly with care providers—based on your loved one’s needs, preferences, and budget—here: https://longtermcarefinder.com/
How to Make the Transition Easier
Transitions in care—whether bringing in help at home or moving to a new setting—can feel emotional for both you and your loved one. It is not just a practical decision. It is a deeply personal one.
Approaching this change with patience, understanding, and open communication can make a meaningful difference.
Helpful Approaches
- Start conversations early, before decisions begin to feel urgent
- Involve your loved one in the process as much as possible
- Visit care options together to build familiarity and comfort
- Focus on safety, comfort, and overall quality of life
- Offer reassurance and ongoing emotional support
These conversations may take time—and that is okay.
For many families, this process unfolds gradually, with small steps that build confidence along the way.
This transition is not about losing independence.
It is about gaining the right level of support to live more safely and comfortably.
Practical Daily Caregiving Tips
Day-to-day caregiving often comes down to small adjustments that make life feel more manageable—for both of you. Simple, consistent routines can reduce stress, improve safety, and create a greater sense of stability.
Everyday Tips That Can Help
- Keep routines consistent to provide structure and predictability
- Allow extra time for daily activities to reduce frustration
- Use adaptive equipment to support safety and independence
- Communicate clearly, calmly, and with patience
- Take breaks when needed to protect your own well-being
If this feels like a lot, you are not alone—many caregivers find that small, steady changes make the biggest difference over time. Even small adjustments can have a meaningful impact.
Over time, these changes can help create a more supportive, manageable daily rhythm—one that benefits both you and your loved one.
As these daily routines take shape, it becomes clear that caregiving is not just about managing tasks—it is about supporting your loved one, and yourself, through every stage of the journey.
Final Thoughts: Supporting Your Loved One—and Yourself
Caring for a loved one with Parkinson’s at home is one of the most meaningful roles you may ever take on.
It is also one of the most challenging.
There will be moments of connection, resilience, and deep love—moments that remind you why you are doing this. And there may also be moments of uncertainty, exhaustion, and difficult decisions.
Both can exist at the same time. You do not have to have all the answers. You do not have to do everything perfectly. What matters most is this:
You are showing up.
You are doing your best.
And that matters more than you may realize.
As your loved one’s needs change, it is okay for the way you provide care to change, too. Support is not a last resort—it is a natural and important part of this journey.
Frequently Asked Questions About Parkinson’s Care at Home
1. How long can someone with Parkinson’s live at home?
Many individuals can continue living at home for years, especially with the right level of support. Parkinson’s care at home often begins with small adjustments and gradually increases as needs change over time.
With the help of family caregivers, in-home care services, and simple home safety modifications, many people are able to remain in a familiar environment longer than they initially expect.
2. What is the biggest challenge in Parkinson’s caregiving?
One of the biggest challenges in Parkinson’s caregiving is adapting to changing needs over time.
As the disease progresses, caregivers often take on increasing responsibilities—particularly related to mobility, medication management, and safety. Balancing these demands while also caring for your own well-being can be one of the most difficult parts of the journey.
3. When should we consider assisted living for Parkinson’s disease?
It may be time to consider assisted living for Parkinson’s disease when care needs begin to exceed what can be safely managed at home. This may include:
- Increased fall risk or mobility challenges
- Difficulty managing medications consistently
- Needing help with most daily activities
- Caregiver stress or burnout
Exploring options early can help families make thoughtful, informed decisions—rather than urgent ones.
4. Is Parkinson’s disease always progressive?
Yes, Parkinson’s disease is a progressive condition, meaning symptoms gradually worsen over time. However, the rate of Parkinson’s disease progression varies widely from person to person.
Some individuals experience slow changes over many years, while others may notice more rapid progression. This variability is why ongoing monitoring and flexible care planning are so important.
5. Is hospice care part of Parkinson’s care?
Yes, hospice care can be an important part of the Parkinson’s care journey, particularly in the later stages.
Hospice care is different from long-term care because it focuses on comfort, quality of life, and symptom management rather than ongoing treatment or rehabilitation. For many families, it provides meaningful support, guidance, and peace of mind during a difficult time.
6. Can someone with Parkinson’s live alone?
In the early stages, many individuals with Parkinson’s disease can live alone safely, especially with small adjustments and support from family or friends.
As symptoms progress—particularly mobility challenges, fall risk, and medication complexity—living alone may become more difficult and potentially unsafe. Regular check-ins, home modifications, or part-time in-home care can help extend independence, but ongoing evaluation is important.
7. What stage of Parkinson’s requires 24-hour care?
There is no single stage that automatically requires 24-hour care, but many individuals need continuous support in the advanced stages of Parkinson’s disease.
This is often when:
- Mobility becomes severely limited
- Assistance is needed for most daily activities
- Cognitive changes or dementia are present
- Safety risks, such as falls or confusion, increase
At this point, families often begin considering full-time in-home care, assisted living, memory care, or skilled nursing.
8. How do you know if Parkinson’s is getting worse?
Parkinson’s progression can be subtle, but certain changes may signal that symptoms are advancing:
- Increased difficulty with walking or balance
- More frequent “off” periods between medications
- Greater reliance on help for daily activities
- Noticeable cognitive or behavioral changes
Tracking these changes over time can help guide care decisions and support more informed conversations with healthcare providers.
9. What kind of care does someone with Parkinson’s need?
The level of care needed depends on the stage of the disease, but Parkinson’s care at home often includes:
- Assistance with daily activities such as bathing, dressing, and meals
- Medication management and scheduling
- Mobility support and fall prevention
- Emotional and cognitive support
As needs increase, care may expand to include in-home care services, assisted living, memory care, or nursing care.
10. Can Parkinson’s patients go to assisted living or memory care?
Yes, many individuals with Parkinson’s disease transition to assisted living or memory care as their needs evolve.
- Assisted living is often appropriate when help is needed with daily activities and medication management
- Memory care may be recommended if cognitive changes or dementia become more significant
These environments provide structure, safety, and specialized support that can be difficult to maintain at home.
